How Privilege Shaped the COVID-19 Pandemic

The March 2020 news about actor Tom Hanks and his wife Rita Wilson’s COVID-19 infections garnered substantial media attention at a time when the pandemic was just beginning its wide reach in other parts of the world. Although the celebrity couple was over 8,000 miles away in Australia when diagnosed, ordinary Americans at home suddenly started to feel closer to this plague than ever before. “Look, even Tom Hanks got it!”
However, Tom and Rita Hanks are not average Americans. Along with enjoying the fame of their global celebrity status, they are among an elite group resourced with top-tier health information and healthcare. Not surprisingly, the two celebrities were among the earliest cases to receive a speedy diagnosis. Meanwhile, so many others were unable to obtain COVID-19 testing.
For centuries, the have and have nots have been distant from one another both socially and spatially. This is also the case when it comes to health and well-being. Medical sociologists and epidemiologists alike have long documented that health and disease are socially patterned across societies throughout modern history. Among the multiple social factors, socioeconomic status is perhaps the most evident. People in the top strata of the social hierarchy enjoy longer life expectancy and lower mortality. When sick, they tend to demonstrate better outcomes in most other health measures (e.g., cancer, cardiovascular disease, Type II diabetes). Another profound factor associated with social status concerns spatial inequalities (e.g., concentrated poverty, fewer health care providers and resources), leading to the unequal distribution of health outcomes across space. Those living in affluent communities have a health advantage compared to others living in less affluent neighborhoods.
Health and disease are not just socially patterned but also originate socially. Sociologists Bruce Link and Jo Phelan theorized that social conditions are arguably a fundamental cause of health disparities, meaning that social determinants (e.g., social class, race) are critical in deciphering what makes certain populations healthy or sick. This is because societal factors establish broader contexts (e.g., social policies, residential and work environments, social networks) that shape individual-level behavioral choices and responses; they are also tightly connected to health-promoting resources and health-detrimental hazards. The centrality of these social factors in conditioning health outcomes goes above and beyond other often talked about individual behavioral and lifestyle choices (e.g., smoking, diet, exercise).
Income inequality in the United States has risen since the 1970s. Life chances for the haves and have-nots are vastly different. Take the case of Los Angeles, for instance (Median Household Income by Census Tract in Los Angeles). The 710-freeway corridor exemplifies how social, economic, and environmental factors negatively impact the most disadvantaged, vulnerable communities in the region. Residents of these communities, most of them being people of color, not only experience high levels of poverty and unemployment but also disproportionate exposure to environmental pollutants and other health hazards, such as air and water pollution, ambient noise, hazardous wastes, substandard housing, and residential overcrowding. Meanwhile, Los Angeles has some of the wealthiest and most privileged communities of the world: Malibu, Beverly Hills, Palos Verdes, just to name a few.
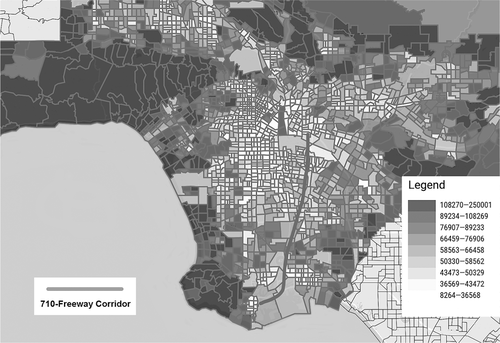
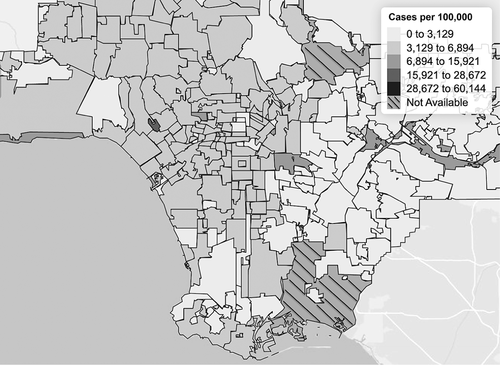
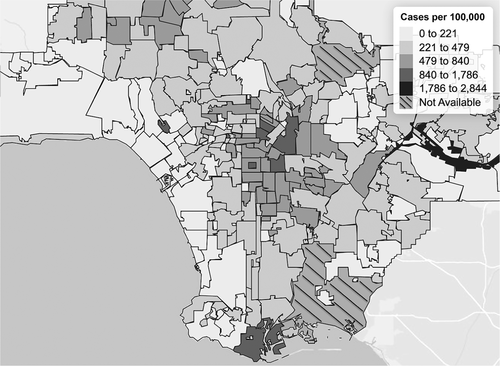
How did these social and spatial inequalities exacerbate health disparities during the early phases of a highly contagious pandemic? The figures above show age-adjusted COVID-19 testing and infection rates per 100,000 residents in the Los Angeles area as of May 21, 2020, according to the LA County Department of Public Health. Not surprisingly, rates of infection (Rates of COVID-19 Infection) largely overlay the income distribution (Median Household Income by Census Tract in Los Angeles) with the 710-freeway corridor being hit particularly hard. Sitting at both ends of the corridor, cities like Vernon and San Pedro have seen confirmed cases multifold to those in more affluent beach communities.
Interestingly, it was not the case in the initial stage of this outbreak. Some reports noted that back in March 2020 many high-income areas of Los Angeles had in fact reported more COVID-19 cases than the rest of the county. This paradox can be explained by a few factors. The wealthy could be disproportionately infected during the initial outbreak as they traveled globally, including business people and students studying abroad. There was also varied access to testing early in the outbreak as many ordinary Americans, front-line healthcare workers included, could not access it. However, this puzzling trend was largely reshaped a few months later, as shown in the figures. Geographic and income disparities in testing narrowed or even disappeared (Rates of COVID-19 Testing) as it became more accessible, while the income-coronavirus correlation also turned from more positive cases being reported among the rich toward those with lower incomes (Rates of COVID-19 Infection).
Statistics aside, what are some of the actual advantages of the rich over the poor during this unprecedented pandemic? As the wealthy had the privilege of early access to COVID-19 testing and subsequent timely diagnosis, it reduced the likelihood of their conditions deteriorating into more harmful stages and afforded them more time for better treatments. Access to early testing also results in a lower likelihood of spreading the virus in their households or communities. Regarding preventive measures, because of their ability to afford more spacious residences and to use personal vehicles for transportation, the rich can limit incidences of close contact with others, including close relatives. Larger living spaces also facilitate more comfortable and effective quarantines. Furthermore, the nature of occupations and lifestyles of the wealthier provides greater flexibility to work from home, thus avoiding unessential outdoor traveling. A Brookings Institute report based on a Gallup survey of 8,572 adults nationwide in late March, for example, identified 71 percent of those at the top quintile of household income ($180,000+) were able to work from home, compared to 35 percent of the lower-middle quintile ($24-$47,000). Racial disparities also emerged regarding work flexibility. White workers were 37 percent more likely than people of color to have jobs that could be performed remotely, according to a McKinsey Global Institute report from April.
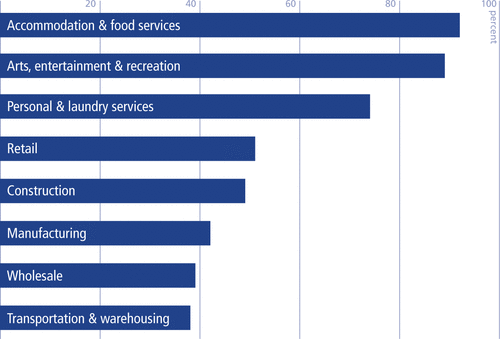
Among the lower-income, how does the nature of their work and vulnerability to economic distress drive their potential exposure to coronavirus? In the months since the pandemic emerged, we have seen skyrocketing unemployment rates with many of the lost jobs in service sectors with lower status and wages. The figure above illustrates the percentage of vulnerable jobs in industries that were significantly impacted nationwide as of mid-April, based on the same McKinsey Global Institute report. It was also found that 86 percent of those vulnerable jobs had an annual pay of less than $40,000, with racial minorities being disproportionately affected. People with lower incomes not only suffer economically; they are also more likely to take on employment with a higher risk of virus exposure or to live with someone who is employed outside their home. Further, essential workers who are fortunate to keep their jobs, such as those working on construction sites or in delivery services, still need to continue traveling and many rely on public transportation.
Not surprisingly, in a study reported by the New York Times, smartphone data tracking fifteen million users nationwide showed the lower-income were much less likely to restrain their quarantine movements. Researchers studying a San Francisco neighborhood also identified 90 percent of those testing positive for COVID-19 could not work from home, with most being low-income and living in households of three or more people. Moreover, the lower-income tend to live in more cramped housing within more densely populated communities. USA Today matched demographic data of 8,500 zip codes from the census with COVID-19 cases collected by 49 state, county, and local health departments during the week of June 15. They reported a higher COVID-19 prevalence in more densely populated neighborhoods with infection rates twice as high in those with over 1,000 residents per square mile. Indeed, the virus can be more prevalent among people who are socially disadvantaged as a result of crowded housing and community deprivation, which also put their family members including elders at much higher risks for a negative COVID-19 outcome.
Advocates have long argued for social justice and community resources to assist local residents with everyday life and well-being. Yet the emergence of COVID-19 reveals again that social disadvantages and unequal distributions of resources continue to drive health disparities. When an unpredicted catastrophe like this suddenly hits, the poor and the disadvantaged are still the bodies of our society suffering more. To reduce these disparities, we need earlier, consistent, and more widespread testing throughout the pandemic available to everyone regardless of social status. We also need social and public policies aimed at providing adequate protections and reducing financial distress, so that lower-wage workers are not at heightened risk for contagious diseases like COVID-19.

Comments 2
Unabis CBD
January 20, 2021Hello! Thank you for such a distal review and analysis of this issue. It seems to me that this is not news for a long time, that rich people live longer and get better quality medical services than the middle class and especially people who live very poorly. I perfectly understand how it is not to be able to afford basic medical services and to postpone the visit to the doctor just because I cannot pay for it. And this is very unfair to people like me. I don't even have the opportunity to live in good health
CANIS LUPUS
March 27, 2021There is nothing new about anything shared in this article. The more specialized and valuable you are to the economic life of your community the more you are paid. The more you are paid the better is you access to anything you need to stay alive. Those with money want to live near people like themselves making it easy for business and professions who want to market services to those well off people. Money grants people two things options and access. Race does not really play into it as much. 'm black as the ace of spades but I have a great job in IT. I work from home. I have all my food and other needs delivered. I have great doctors and awesome medical insurance.
COVID19 has been nothing much more than an annoyance to me because of the privilege that comes with wealth and a great paying career. My black skin opens few doors. My $62 per hour career opens all the doors I need to survive COVID19.